Abnormal Uterine Bleeding in the Reproductive Years
Pathogenesis, Investigation, and Clinical Management
Malcolm G. Munro MD, FRCS(c), FACOG
Clinical Professor, Department of Obstetrics & Gynecology
David Geffen School of Medicine at UCLA
Kaiser Permanente, Los Angeles Medical Center
Los Angeles, California, USA
Abnormal uterine bleeding (AUB) in the reproductive years is a problem that impacts uncounted millions of women worldwide. Bleeding that women consider excessive or unacceptable and for which they seek care covers a broad range of volume and predictability. The diagnosis of ‘clinically significant’ bleeding is not limited to that which results in anemia; any bleeding of uterine origin that adversely impacts quality of life is indeed ‘abnormal’. For example, a woman without anemia but with bleeding of unpredictable onset may be unwilling to participate in routine activities, may require continuous access to pads and/or tampons, and may fear social activity or sexual relationships because she always perceives that she is on the precipice of a period.
It is important for the clinician to remember that chronic AUB rarely is a life-threatening circumstance and that, for the vast majority of women, appropriate counseling will allow them to make their own informed decision. The decision is made in the context of a strategy that is appropriate to her condition, her desires regarding current and future fertility, and her sense of perceived side effects and risks.
So how can the electronic version of this book help you, the provider, help the women afflicted with acute or chronic AUB? First of all, for navigation, the full Table of Contents is found on the “Sitemap,” and the tiles elsewhere on the screen can get you to the various sections – how these look on your screen will vary depending on the device that you are using at the time – personal computer, tablet or smartphone.
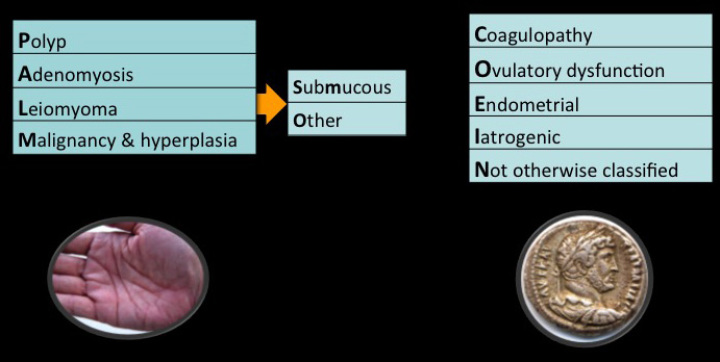
The first three sections support a better understanding of the physiology of normal menstruation, the known pathogenesis (“causes”) of abnormal bleeding, and the design of the FIGO systems for the nomenclature of symptoms and classification of causes of AUB. This sets the stage for understanding the ‘whys and hows’ for identifying and investigating women with AUB with the descriptions and resources of the “Investigation Toolbox”, aided by the “Image Library” and some downloadable tools for both patients and clinicians. Here the importance of the structured menstrual history and appropriate uterine imaging techniques are emphasized along with the requirement of the clinician to integrate the results, which often include both clinically relevant and asymptomatic findings. This process allows for the development of a complete menu of treatment options that empowers the woman presenting with AUB to make choices consistent with her perceptions, needs, and goals, particularly with respect to the integrity of her reproductive tract. The “Management Toolbox” should provide you, the reader, with medical and surgical options for each of the PALM-COEIN categories, along with a selection of videos for brief descriptions of technique.
And what about evidence? As with any branch of medicine, the quality of evidence supporting our decisions regarding investigation and therapy varies greatly – from abundant randomized controlled trials (RCTs) with supportive systematic reviews and meta-analyses, to an evidence wasteland barely populated with case reports. Fortunately, Sackett has provided us with, in my opinion, the best definition of evidence-based medicine and one that applies to all clinical conditions.(1)
“The conscientious, explicit, and judicious use of current best evidence when making decisions about the care of individual patients”
Each of the words “conscientious”, “explicit”, and “judicious”, are important to the concept of EBM. The conscientious clinician should acquire knowledge of the case-related external evidence for each and every patient in a careful and meticulous fashion that is facilitated by the wealth of available electronic resources such as the Cochrane Library, MEDLINE, and other sources. In some instances, there is no published external evidence applicable to the clinical presentation or condition, a circumstance where the best available evidence will be the experience of the clinician. Whatever the source, the therapeutic options and decisions should be made in the context of the best available external evidence, explicitly stating why that evidence does or does not apply. It is this clinical decision, the judicious application of the best available evidence, which is totally reliant on the clinical expertise of the practitioner. This resource can be aided but never replaced by external evidence. At the bottom of the sections of this electronic “book” are reference lists hyperlinked to PubMed, where the full abstract can be found – and, if you have personal or institutional access, you will be able to get to the full reference.
Finally, remember that effective clinical medicine requires the creation of a relationship with your patient that is established by effective communication. The ability to obtain an accurate history is a skill that cannot be replaced by evidence, tests, drugs, or devices, and without it, the clinician and patient will walk a precarious path. This approach could be summed up in a quote often attributed to Sir William Osler, who said, “ Listen to the patient – she is trying to tell you what is wrong.”
Malcolm G. Munro MD
Los Angeles, California
Reference